
There are many ways to test municipal wastewater for signs of the virus that causes COVID-19, but scientists in Houston have determined theirs is the best yet.
A study led by environmental engineer Lauren Stadler of Rice University’s Brown School of Engineering with the aid of the City of Houston Health Department and Baylor College of Medicine compared five processes used by labs around the country to concentrate samples and find the virus in wastewater from six Houston plants.
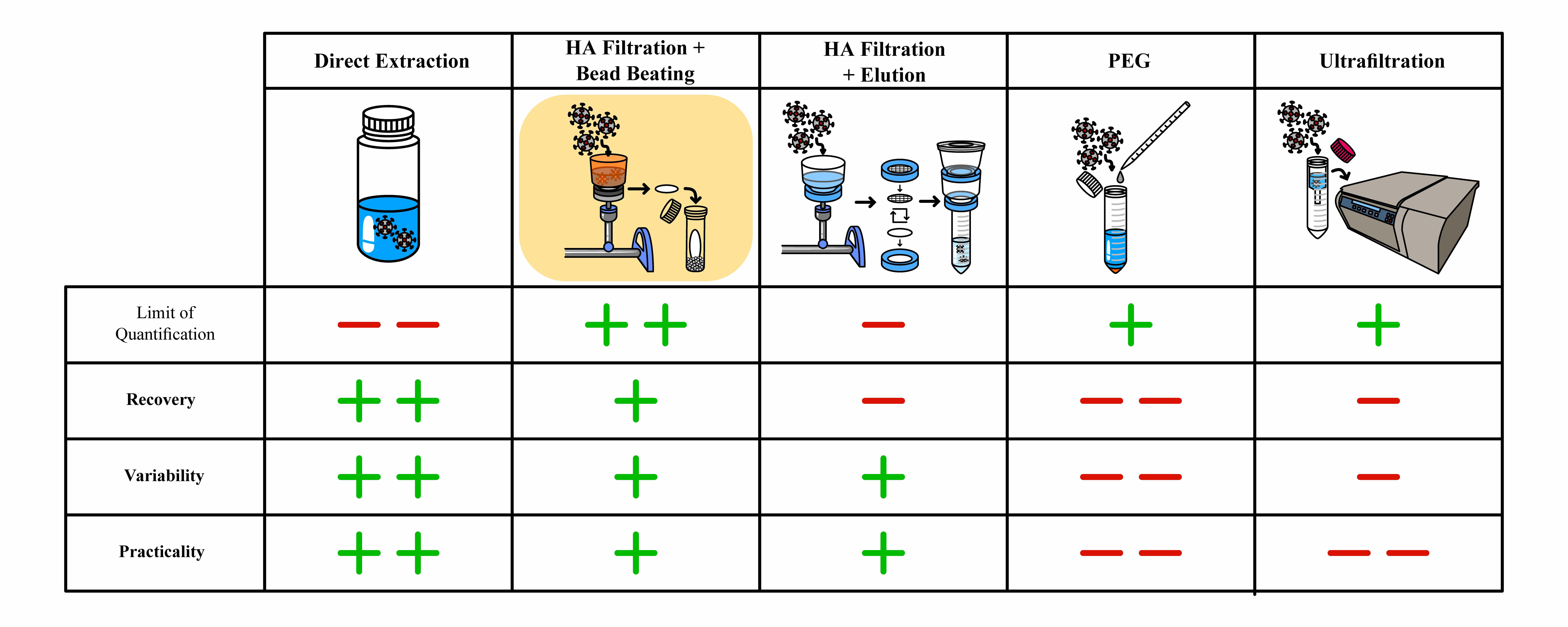
The process employed at Rice and now Baylor, called “electronegative filtration with bead beating,” proved the most sensitive to signs of the virus as well as the most cost-effective.
The study appears in the Elsevier journal Water Research.
There is no standard test, according to the study, but all of the processes — including electronegative filtration with elution, ultrafiltration, precipitation and direct extraction — are effective to a degree.
“The virus is extremely dilute in wastewater, so we need a way to concentrate it,” Stadler said in explaining the Rice process. “First, we add salt to the wastewater sample to enhance adsorption of the virus to the electronegative filter. After filtration, we physically beat the filter with glass beads to release the virus into a lysate. Even though this process might break up the virus, we only detect tiny fragments of its RNA genome to quantify it.”
Established in spring 2020, the Houston coalition was on the leading edge of what became a nationwide effort to find the SARS-CoV-2 virus in wastewater. The technique quickly proved able to anticipate COVID-19 outbreaks and allowed health officials to ramp up testing where needed.
“When we started testing, Baylor was using a different method,” Stadler said. “That gave us the opportunity to do a lot of head-to-head comparisons about which method to use. And that led us to want to do a more comprehensive evaluation of several methods that were commonly being used to concentrate SARS-CoV-2 in wastewater by other groups around the world.
“There’s not one right method, but we wanted to be sure we considered other options,” she said. “Our recommendation and final method selection was based on finding a balance between sensitivity, throughput and cost.
“The method we selected originally turned out to have the lowest detection limit, while also being relatively high-throughput and cost effective,” Stadler said. “Baylor switched over to the same concentration method as a result, which gave us confidence that we were truly generating the best possible data for the city.”
The Houston researchers hope the study will guide municipalities around the world that have, or are considering, their own wastewater testing labs.
“A lot of major cities are already doing this, and there are now statewide programs emerging in Michigan, Wisconsin, North Carolina and a few others,” Stadler said. She noted the Houston labs are already looking for COVID mutations. “We’re doing research on sequencing wastewater samples to be able to detect highly transmissible variants circulating in the community,” Stadler said.
That the study even happened is a bonus, considering the workload for Stadler’s Rice lab and counterparts at Baylor and the Houston Health Department. Since ramping up in mid-2020, the labs have analyzed hundreds of samples a week from the city’s 39 wastewater plants. Since then, Houston has added testing points at dozens of nursing homes, schools and other critical locations.
“The city is planning to expand the number of stations to get zip code-level information, and we’re working with them to analyze that data,” Stadler said. “Someday, it could be a tool to look for a panel of viruses, not just this one.”

