
A newly published study by the University of South Florida Health (USF Health) and Tampa General Hospital (TGH) shows that monoclonal antibodies (MABs) work well in reducing COVID-19 related emergency department visits and hospitalizations when given early to high-risk patients. If used under FDA guidelines, the researchers suggest, this treatment can ease the pandemic’s continuing burden on patients and on limited health care resources.
The collaborative study was published June 4 in Open Forum Infectious Diseases.
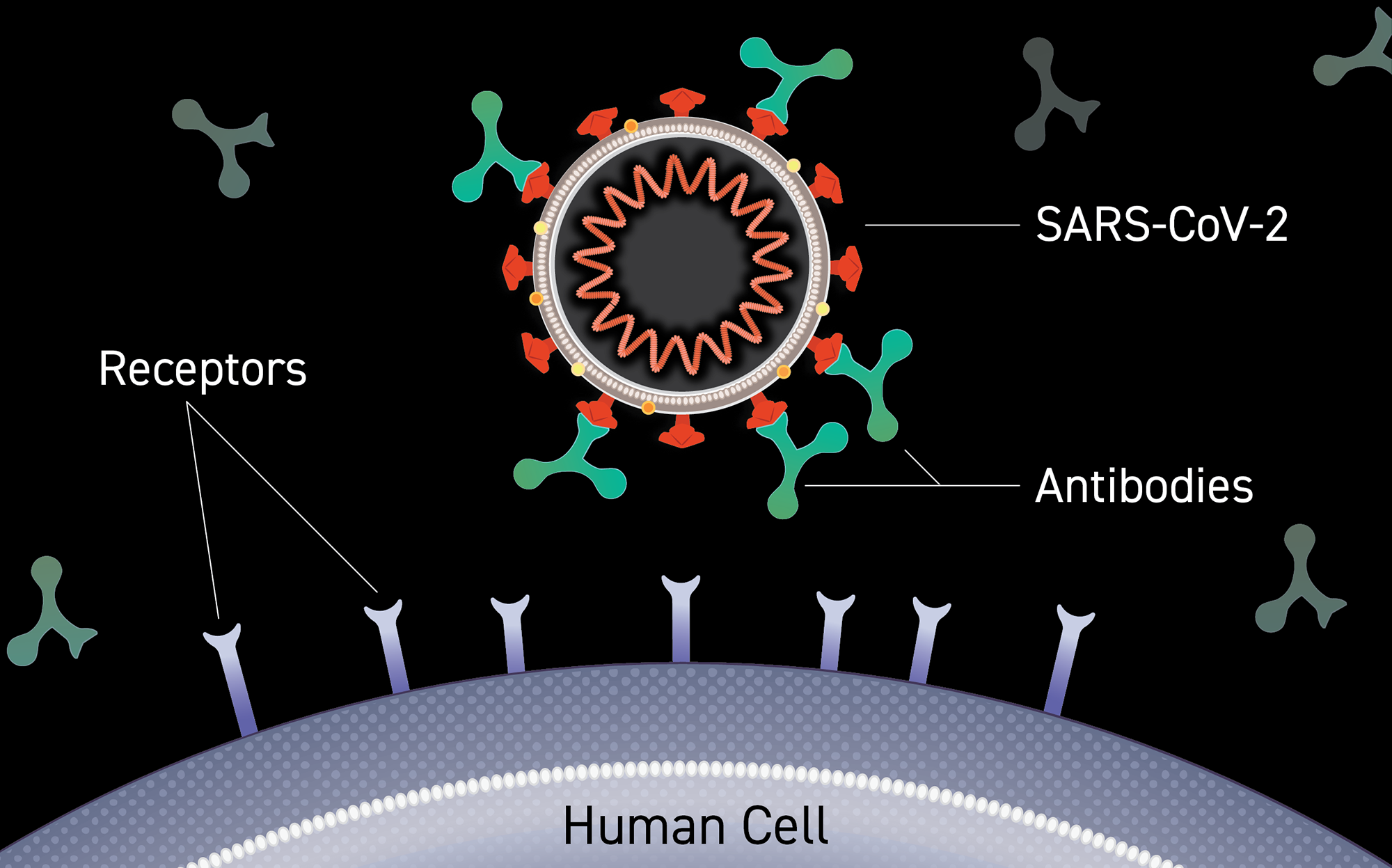
Investigational monoclonal antibody therapies, administered intravenously, are specifically designed to block infection by SARS-CoV-2, the virus that causes COVID-19. The FDA has granted emergency use authorization (EUA) of MABs in outpatients with mild-to-moderate COVID-19 at increased risk of developing severe disease. Such high-risk patients are prone to hospitalizations, mechanical ventilation and other complications, including death from coronavirus.
“While the emphasis now is rightfully on getting more vaccines in arms, thousands of people in the U.S. are still infected with COVID-19 every day and a significant number suffer serious complications,” said the study’s senior author Asa Oxner, MD, associate professor and vice chair of the Department of Internal Medicine, USF Health Morsani College of Medicine.
“Unfortunately, only a fraction of those outpatients eligible for monoclonal antibodies receive them,” Dr. Oxner said. “We hope results like ours reinforce to the public and health care providers the importance of targeting timely monoclonal antibody treatment to this high-risk patient population to help minimize stress on health care systems during the COVID-19 pandemic.”
Limited clinical trials previously indicated that MABs work best when given soon after diagnosis. But this USF Health-TGH collaborative study was one of the first to evaluate the practical effectiveness of MABs when administered exclusively to patients deemed at high risk for progression to severe COVID-19. The FDA defines medical conditions and factors that place adults and children age 12 or older at higher risk for COVID-19, including older age (65 plus), obesity, diabetes, immunosuppressive disorders or treatment, chronic lung disease and cardiovascular disease, to name a few.
The academic medical center’s retrospective study, conducted Nov 18, 2020, to Jan. 5, 2021, included high-risk outpatients with a confirmed COVID-19 diagnosis, all experiencing mild-to-moderate symptoms for 10 days or less. A group of 200 patients received one of two MAB therapies (a single infusion) – either casirivimab/imdevimab, a combination drug made by Regeneron, or the medication bamlanivimab made by Eli Lilly. This treatment group was compared against a control group of 200 randomly selected outpatients who declined or were not referred for MABs during the same period.
Among the findings:
-
- – Overall, patients treated with the MABs were significantly less likely to be hospitalized or visit the emergency department (13.5%) than the control patients (40.5%). These results remained significant when comparing the individual monoclonal antibody therapies against the control group.
– No deaths were reported in the MABs-treated group, compared to 3.5% in the control group.
– Patients treated with MABs within six days of symptom onset were significantly less likely to be hospitalized or visit the emergency department (7.7%) than those treated after six days (28.1%). The study data indicated MABs are best given within seven days of initial symptoms to reduce the odds of hospitalization within 29 days of infusion.
“Reflecting on our findings, it would be prudent to consider decreasing the FDA eligibility window for MABs to within seven days of symptom onset,” the study authors write. “These medications are a relatively scarce resource, and it would be practical to administer them to patients who are likely to see the most benefit.”
COVID-19 has strained financial and personnel resources across all health systems, with the Florida Hospital Association estimating total losses of $7.4 billion from the beginning of the pandemic through August 2020. The study authors conclude that maximizing the use of monoclonal antibody therapies under EUA guidance has the potential to “keep high-risk COVID-19 patients out of the hospital and reduce the negative impact on the health care system.”

