
Perhaps the most important question now about COVID-19 is the degree to which a prior infection protects from a second infection by the new coronavirus. This affects vaccine development and herd immunity and is something for each of us to consider as antibody tests are now available.
I am a physician scientist and have a Ph.D. in microbiology as well as an M.D. My clinical specialty is internal medicine and I subspecialize in infectious diseases. I am working on one approach to COVID-19 vaccination while also caring for hospitalized patients.
Here are my responses to common questions surrounding tests and what they can tell you about immunity.
What are the different types of COVID-19 tests?
The nasal swab PCR test that we have all seen in the news, and which 22 million of us in the U.S. have used, reflects whether you are currently infected with the new coronavirus that causes COVID-19. This test detects the genetic code of the SARS-CoV-2 virus in your body. If you have a positive nasal swab PCR result, you not only have the infection, but you are potentially infectious and should stay isolated until recovered.
In contrast, the antibody test determines if you had COVID-19 sometime in the past. It is measuring your body’s immune response to the infection, something that occurs over days to weeks after the infection starts. The antibody can appear after the infection is resolved, or even while you are still infected.
Can the immune system cure COVID-19?
The answer here is a resounding yes.
In all but a tiny percent of cases – maybe 1 in 100 – the immune system naturally eliminates SARS-CoV-2 from the body. This is very encouraging for vaccine development, as making an effective vaccine should be much easier than for HIV or hepatitis C virus, for example, where the immune system often (for hepatitis C) or almost always (for HIV) fails. SARS-CoV-2 differs from these two viruses because it has a so-called proofreader gene that prevents mutations from being introduced during viral replication.
Do antibodies work to prevent a new coronavirus infection?
The answer here is maybe.
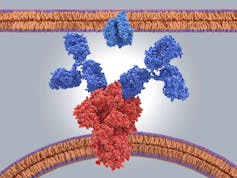

We know that in a test tube antibodies against the virus can neutralize it. That is, they can prevent the virus from entering into a human cell and causing an infection. But not every antibody is equally capable of preventing the virus from causing an infection.
The very best antibodies are ones that neutralize the receptor binding domain of the new coronavirus spike protein that attaches to the host cell’s ACE2 receptor. The RBD is on the tip of the spike protein and is the part of the spike that touches ACE2. Antibodies against RBD block the very first step of viral infection, which is when the coronavirus attaches the human cell membrane.
If my antibody test is positive, am I immune?
Another maybe.
Clouding the interpretation of a positive antibody test is that we do not yet know if antibodies against RBD make people immune. We also don’t know how much of this antibody against RBD is needed to ensure protection.
Complicating things further is the fact that not all of the antibody tests for COVID-19 measure antibodies against RBD. Some tests measure antibodies against parts of the virus that are not needed for cell entry. These antibodies that are not against the RBD will recognize the virus but will not block it from infecting human cells and triggering viral infection.
So only antibodies that block the spike protein from connecting to the ACE2 receptor are guaranteed to provide immunity. And only antibody tests that measure the amount of these antibodies can predict immunity.
We will have a better understanding of the ability of antibodies against the RBD to protect from infection this summer when large phase III vaccine studies start. This is because these vaccines are designed to make antibodies against the RBD.

Should I get an antibody test?
If you are curious whether you had COVID-19 in the past then yes, it makes sense to be tested. Be aware, however, that some of the tests to date have shown a high number of false positives.
If you do have antibodies, do not assume you an invulnerable to the new coronavirus; you might be just as susceptible as someone who has no antibodies.
So even if you do have antibodies, wearing a mask indoors and maintaining social distancing is still key for all of us as we cope with the continued threat from this pandemic.
William Petri, Professor of Medicine, University of Virginia
This article is republished from The Conversation under a Creative Commons license.

